Sleep Studies
What is a polysomnogram (PSG)?
A polysomnogram or PSG is a recording of multiple physiologic parameters during sleep. It is most often used for the diagnosis of sleep disordered breathing, such as obstructive sleep apnea. Other common uses for PSG include titration of nasal continuous positive airway pressure (CPAP) for treatment of sleep apnea, diagnosis of periodic limb movements during sleep, and classification of problematic sleep-related behaviors such as nocturnal seizures or parasomnias (i.e. sleepwalking, sleep terrors, and rapid eye movement behavior disorder).
What happens during a PSG?
You will typically be asked to arrive at the sleep laboratory between 7-8 pm and complete a questionnaire about your activities on the day preceding the study. A technician will then work with you to review the testing procedure and set up your monitoring equipment for the overnight recording.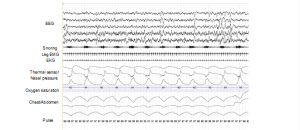 Wires attached to small metal disks called electrodes will be glued to your scalp, so that brain waves can be monitored (electroencephalography or EEG) to help us determine your stages of sleep. Similar metal disks will be attached next to your eyes, next to your chin, and on your legs to give us information about muscle movement. A single electrocardiogram (EKG) lead is used to identify your heart rate/rhythm. Airflow is measured by pressure and temperature sensors that rest under the nose. A small microphone will be placed on your chest to record snoring. A pulse oximeter on your finger will monitor your oxygen saturations. Finally, elastic bands around your chest and abdomen tell us about your respiratory efforts. All of this equipment is very lightweight and designed to be as comfortable as possible when you sleep. A sample PSG recording is shown here.
Wires attached to small metal disks called electrodes will be glued to your scalp, so that brain waves can be monitored (electroencephalography or EEG) to help us determine your stages of sleep. Similar metal disks will be attached next to your eyes, next to your chin, and on your legs to give us information about muscle movement. A single electrocardiogram (EKG) lead is used to identify your heart rate/rhythm. Airflow is measured by pressure and temperature sensors that rest under the nose. A small microphone will be placed on your chest to record snoring. A pulse oximeter on your finger will monitor your oxygen saturations. Finally, elastic bands around your chest and abdomen tell us about your respiratory efforts. All of this equipment is very lightweight and designed to be as comfortable as possible when you sleep. A sample PSG recording is shown here.
After your equipment is in place, you will be able to read, watch TV, or otherwise relax until you are ready to go to sleep. A bedroom in the sleep laboratory is typically designed like a hotel room with a comfortable bed and bathroom facilities. When you are ready to fall asleep and start the study, the technician will perform some basic calibrations of the equipment by asking you to look in different directions and complete some breathing activities. After the lights are turned off, the technician may come into your room to ask you to change position to assess the effect that this has on sleep disordered breathing. If you qualify for the use of CPAP to treat sleep apnea, you may also participate in an overnight titration to find the best pressure setting for the machine. The study is usually finished between 6-7 a.m. and the technician will help you remove all of the monitoring equipment at that time.
How should I prepare for a PSG?
In general, you should perform your usual daily activities leading up to a PSG. You will only need to bring clothes and personal hygiene items for an overnight stay. All medications should be either taken prior to coming in for the study (preferable) or brought with you – no medications are available at most sleep laboratories. If you feel that you might have trouble falling asleep in the sleep laboratory, talk with your physician about prescribing a sleep aid before the test. More specific questions can be addressed by your sleep laboratory or physician prior to the study. Accommodations for caregivers and other special needs can usually be provided.
Are there other types of sleep studies?
We offer complimentary overnight oximetry studies to screen for sleep apnea at select offices. Our North Metro Center for Sleep Medicine also participates in an accredited home sleep testing program through the American Academy of Sleep Medicine; your sleep specialist will determine if this type of sleep study is appropriate for you. A multiple sleep latency test (MSLT) is used to evaluate for excessive daytime sleepiness, such as is seen in narcolepsy and related disorders. This test involves 4-5 daytime nap opportunities at 2-hour intervals, usually starting 2 hours after waking up in the morning following PSG.
Locations/Contact Information:
Evaluations at the North Metro Center for Sleep Medicine, including a comprehensive sleep history and examination, are performed by Dr. Jason Cornelius, and Jamie Witt, PA-C. Your health care professional can arrange for a consultation by contacting us at our Maple Grove office.
Minneapolis Clinic of Neurology – Maple Grove Office
9645 Grove Circle North, Suite 100
Maple Grove, MN 55369
763-302-4114
Laboratory-based sleep studies and pick-up of home sleep testing equipment are provided through the North Memorial Sleep Health Center. This facility is accredited through the American Academy of Sleep Medicine and features state-of-the-art diagnostic equipment in comfortable surroundings. If a sleep study is recommended, our office will assist you with scheduling.
North Memorial Sleep Health Center
13800 83rd Way N, Suite 102
Maple Grove, MN 55369
(763) 581-5050
North Memorial Sleep Health Center is located on the northeast corner of I-94 and Weaver Lake Road. Free parking is available.


